Authored By:

How technology is reshaping the clinical pathway and redefining the patient experience
The pandemic continues to add pressure to healthcare organizations across the U.S. From increased pricing for drugs and equipment to recruitment challenges to the great resignation, healthcare CFOs, HR and quality managers, and department directors are left wondering if there is an end in sight. Sadly, it may get worse before it gets better.
According to a May 11, 2022 report from McKinsey , the U.S. could see a deficit of 200,000 to 450,000 registered nurses available for direct patient care by 2025 if there are no changes in current care delivery models.

To put that into perspective, McKinsey estimates that for every 1 percent of nurses who leave direct patient care, the shortage worsens by about 30,000 nurses. The impact this will have on care delivery and the patient experience is concerning, especially when considering the aging population.
By 2030, 71 million Americans (about 20% of the U.S. population) will be 65+, a demographic known to have complex health problems, chronic illnesses, and disabilities. If things don’t change in the U.S. healthcare system, there will be more patients than nurses to care for them.
Aggressive international recruiting brings with it its own set of concerns and challenges. It’s a short-term fix to a long-term problem.
While filling the nurse pipeline is one solution, it takes three to four years to train a nurse. The U.S. would need to double the number of new graduates entering and staying in nursing every year for the next three years. The challenge is there aren’t enough nursing programs and educators to handle the influx. An analysis of graduating nurses shows the decline – dropping from an increase of 4 percent in 2019 to only 1 percent in 2020, far short of what’s needed to support our healthcare system.
And that’s just part of the healthcare crisis problem.
The Financial Impact of COVID on Healthcare Organizations
According to the Centers for Disease Control and Prevention, there have been more than 97 million COVID-19 cases, 1.06 million deaths, and more than 21 million hospitalizations in the U.S. This has placed an enormous strain on healthcare workers. When combined with rising costs for medications, equipment, etc., these numbers have resulted in billions in lost revenue.
More than 33% of hospitals are operating on negative margins, according to the American Hospital Association.
Many can’t get the nursing staff needed to increase surgeries and cover the budget shortfall. Typically, when there is a staffing shortage, the budget used not paying salaries can be reallocated for increased costs; however, hospitals were paying travel nurses to help address the staffing shortfall.
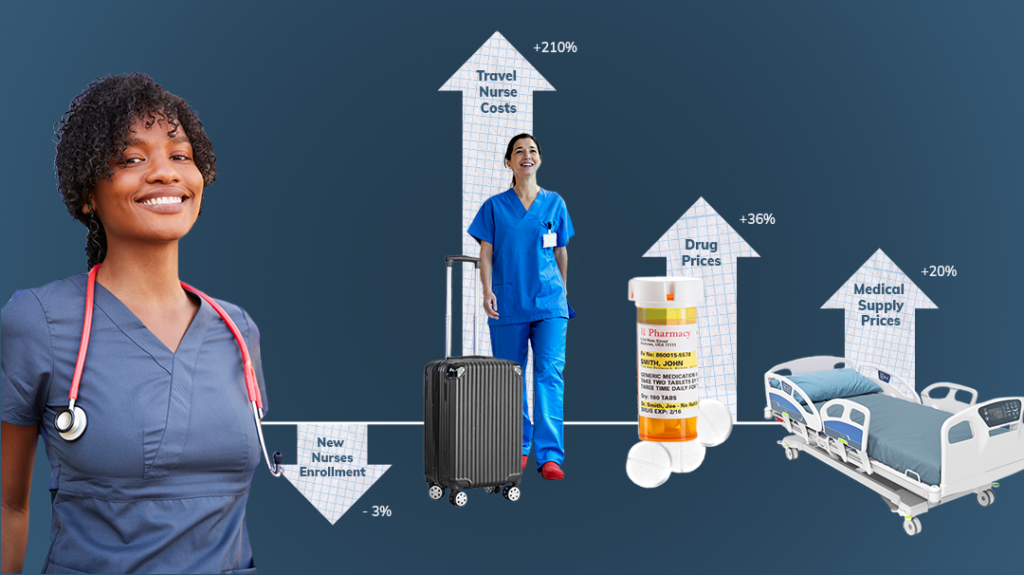
In 2019, hospitals spent a median of 4.7 percent of their total nurse labor expense for contract travel nurses. That number skyrocketed to 38.6 percent (median) in January 2022. Contract labor rates skyrocketed 213 percent compared to pre-pandemic levels. Medical supplies and drug expenses were up 20.6 and 36.9 percent, respectively.
When considering the financial impact these factors have had on healthcare organizations, it becomes clear that adding headcount isn’t going to fix the problem.
Solutions for the Healthcare Crisis
Digital Transformation
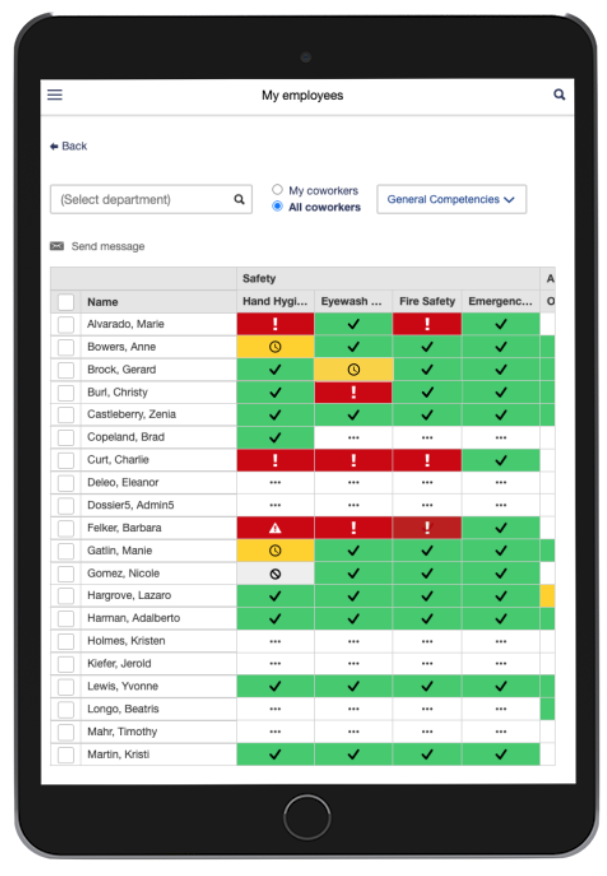
Digital transformation in healthcare translates to the ability to serve patients better digitally. It means adopting technologies to improve workflows, efficiency, and patient care. One area that could easily be improved involves shifting from paper-based competency management (for orientation packets, skills check-offs, and annual mandatories to name a few) to a digital competency management platform.
Only 20 percent of what staff needs to know is captured in learning management systems. The other 80 percent is competencies – knowledge, skills, judgment, and behaviors. Information that is critical to their roles, but currently captured on paper and stored in three-ring binders. This paper-based approach creates enormous waste and inefficiencies, further draining healthcare resources.
Antiquated Processes Hemorrhage Resources
Consider the waste in paper-based competency management:
- Wasted time
- Chasing papers and/or redoing lost paperwork
- Updating competency plans for individuals, departments and facilities, and the time spent printing out plan changes and updating binders – hours upon hours of time when hundreds of staff are involved
- Cost of paper, binders, storage areas
- Duplication of competencies from one department to another because of the lack of visibility
- Inability for those onboarding or going through training to easily and clearly see where they are in the process, what’s required of them, etc.
In the current paper-based competency management environment, when changes are needed, time is spent going into each individual’s plan, making changes, printing the changes, finding the staff member, finding the person’s binder, switching out the plans, putting the binder back, etc. When you multiply the time spent doing this by the number of staff members involved, the need to go digital becomes clear.
The Care Team of the Future
To improve patient outcomes by delivering better quality and focusing on safety, schedulers need to know and be able to track that team members have the skills, knowledge, judgment, and behaviors required for what’s expected of them. And they need that information at their fingertips – not spread across a hospital in lockers, on desks, and in storage rooms.
When plans are digital:
- Plans are created and pushed to appropriate staff in minutes
- Updates happen with a few clicks
- Reminders are easily sent to those falling behind
- Reports for regulatory agencies occur in real time
If you are ready for the next step, request a 15-minute meeting.