Contributor: Ryan Owens
PharmD, Editorial Director, Special Publishing American Society of Health-System Pharmacists (ASHP)
What we can do to reduce adverse drug events and medical errors.
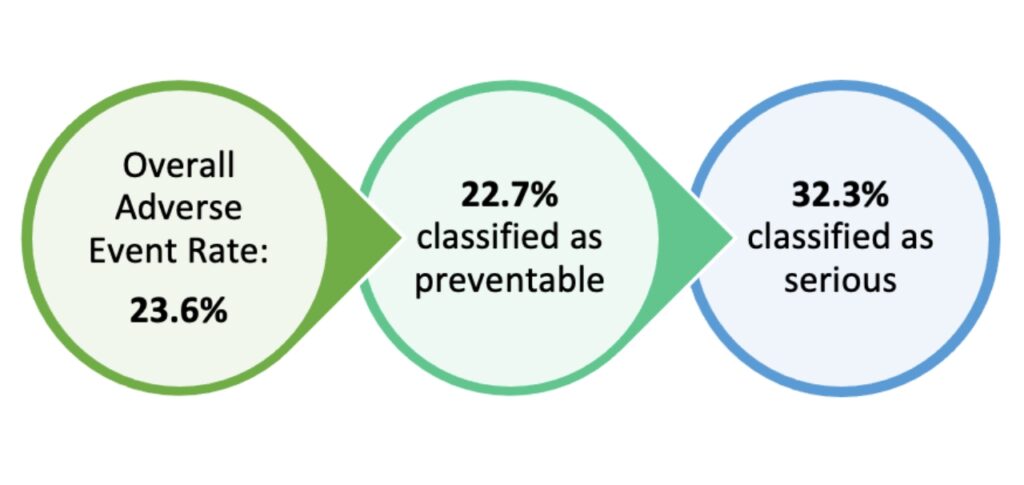
Despite advancements in healthcare technology and medication safeguards, medical errors continue to occur at a high rate within health systems. A recent study by Bates et al published in the New England Journal of Medicine helped quantify the landscape of medication safety within inpatient sites.1 Bates and colleagues analyzed data from 11 Massachusetts hospitals and over 2,800 random admissions during 2018. Key findings of the study are noted in Figure 1 below.
The most common type of adverse event was an adverse drug event, followed closely by surgical or other procedural events. The authors also found that adverse events were higher among older patients and men. Event rates were noted to be higher among larger hospitals as well.
Figure 1: Key Findings
The study did have some limitations, such as a low population of Medicaid and uninsured patients and study sites limited to one geographic area, which could limit its applicability to other hospitals. However, it is one of the more comprehensive studies to critically examine adverse events from multiple sites as a follow-up to findings from the landmark Harvard Medical Practice Study in 1991.2
The findings of this study indicate that individual hospitals and the healthcare system at-large continue to have room for improvement regarding patient safety and delivery of care. The authors noted a few key elements are essential to help enhance safety standards within an organization and include:
Accurate and appropriate measurement of adverse events for organizations, which can often be complex to achieve, is an initial step to improving safety.
Appropriate safety culture
Dedicated leadership
Regular, ongoing competency training can help staff remain up to date in their knowledge and skills by educating on the latest guidelines and standards of care.
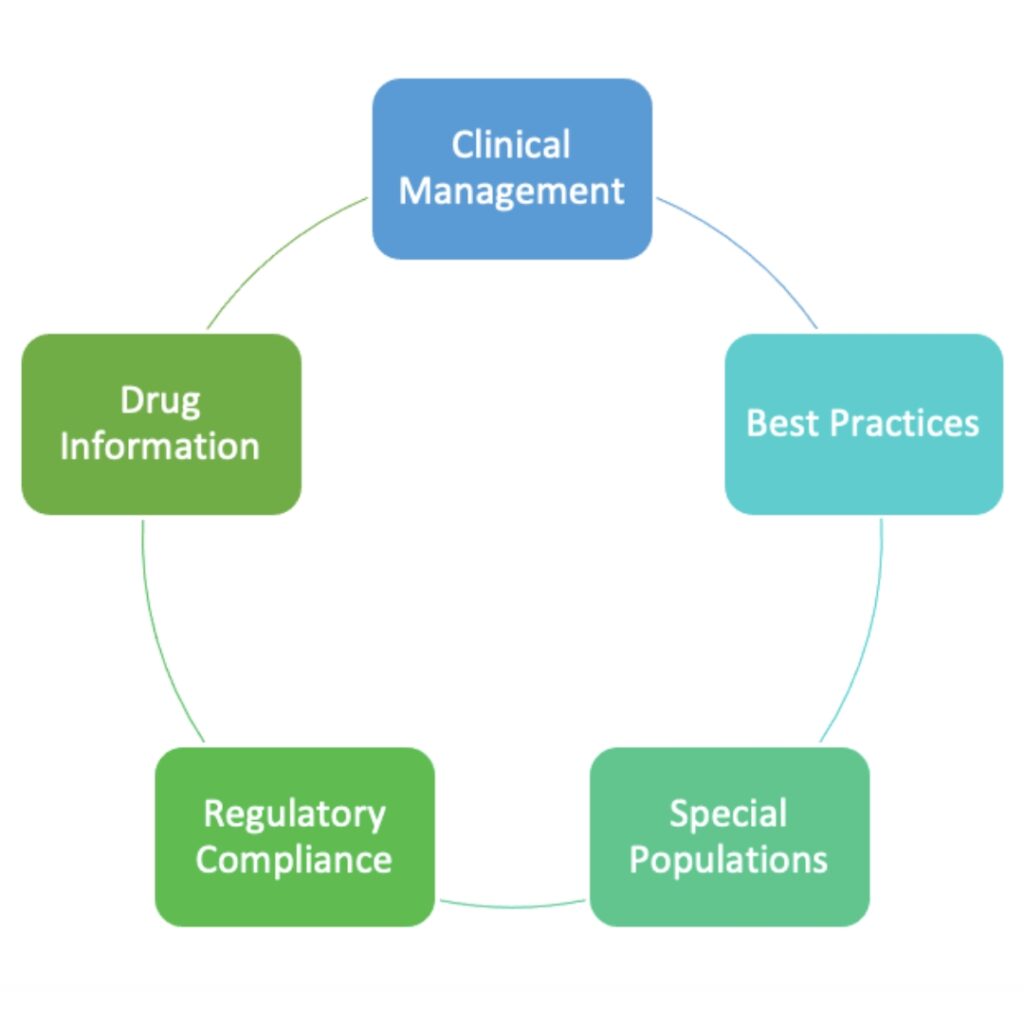
Given the implications to overall patient care, improving safety should be a top priority for organizations. While a multi-targeted approach for improvement should be included, one recommended avenue can be through continuous staff education and training. Regular, ongoing competency-based training can help staff remain up to date in their knowledge and skills by educating on the latest guidelines and standards of care. Examples of potential competency-based training topic areas are included in Figure 2.
Ensuring staff are competent in specific areas related to their roles and responsibilities can help elevate the care provided to patients. Competency-based training also allows staff to receive a refresher on fundamental topics and assimilate new knowledge on changes in treatment recommendations. Training can also be tailored to the specific practice area and individual needs of a staff member.
Figure 1: Competency-based Training Topics
A Whole New View On Competency
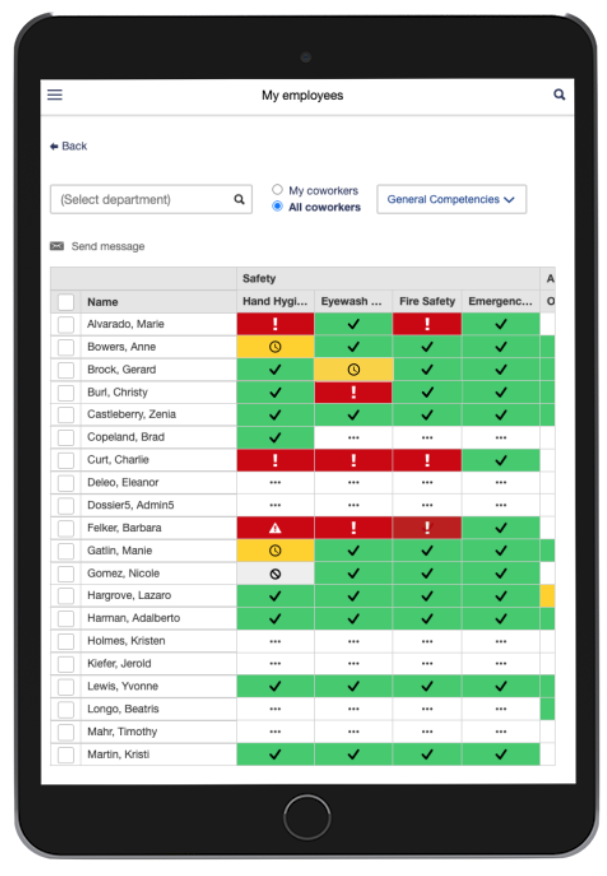
Competency-based training can be a valuable tool to not only help improve safety, but also provide continuous professional development for staff. The American Society of Health-System Pharmacists (ASHP) have developed a full suite of digital competency trainings and assessments to manage and monitor competency completion among pharmacist and pharmacy technician staff. With Dossier’s robust competency platform and the power of ASHP’s Competency Assessment Centers content, you’ll have the perfect formula for a successful pharmacy.
To learn how ASHP’s Competency Assessment Centers content and Dossier’s competency management tool can help your organization, schedule a quick demo.
References
Bates DW, Levine DM, Salmasian H, et al. The safety of inpatient healthcare. N Engl J Med 2023; 388:142-153.
Brennan TA, Leape LL, Laird NM, et al. Incidence of adverse events and negligence in hospitalized patients — results of the Harvard Medical Practice Study I. N Engl J Med 1991;324:370-376.